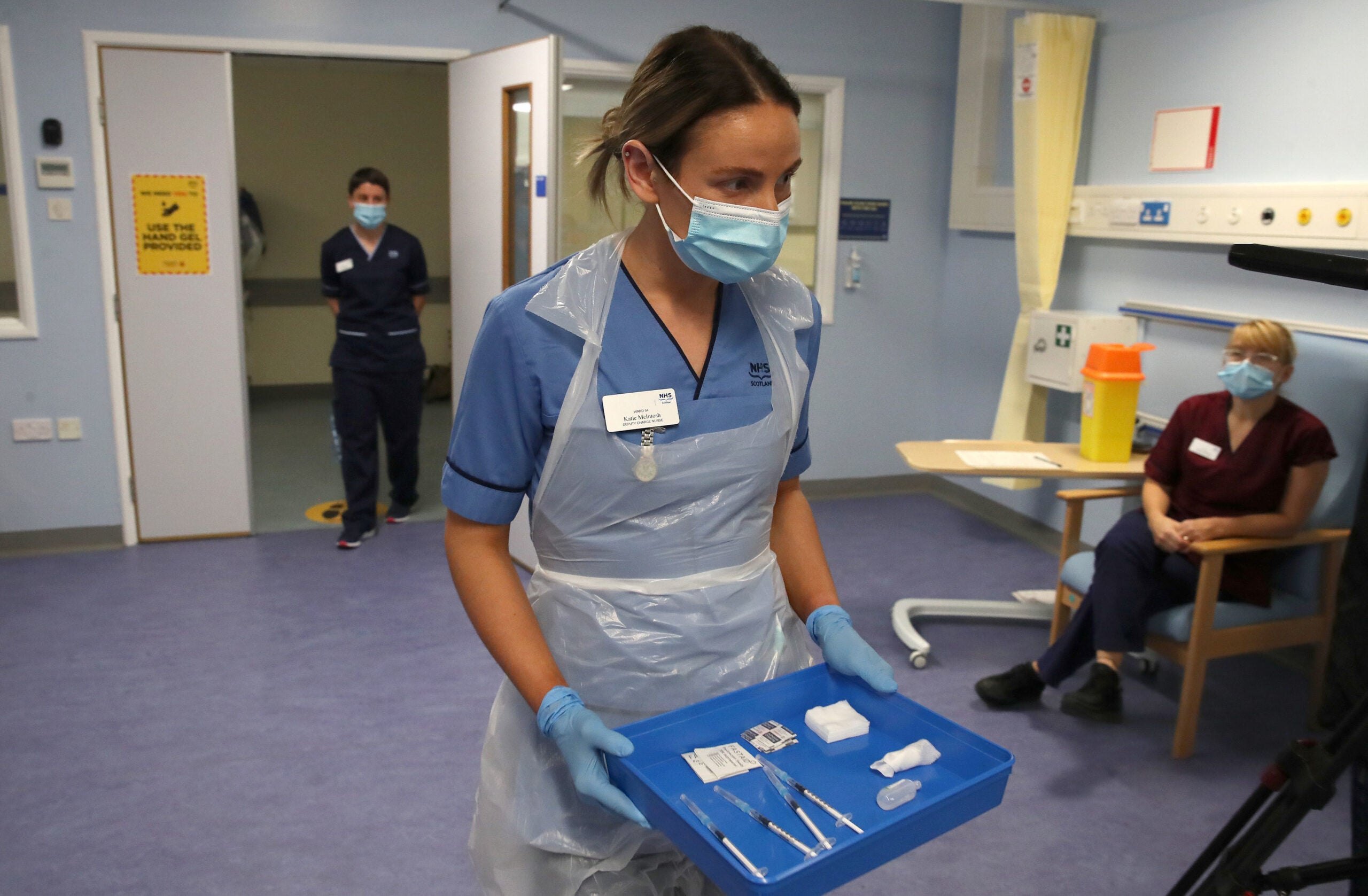
Less than a week after the UK’s Medicines and Healthcare products Regulatory Agency (MHRA) temporarily approved the world’s first Covid-19 vaccine – Pfizer/BioNTech’s BNT162b2 – the UK’s National Health Service (NHS) began administering the vaccine to NHS staff and patients aged over 80 years. Therefore, Tuesday 8 December will go down in history as the first time a Covid-19 vaccine had ever been administered to patients outside of a clinical trial.
However, less than 24 hours after the beginning of the UK’s vaccine roll-out, Pfizer/BioNTech’s Covid-19 vaccine has already been greeted with a safety concern.
Allergic reactions associated with Covid-19 vaccine, BNT162b2
After two NHS workers who received the Covid-19 vaccine experienced symptoms of a severe allergic reaction, the MHRA has recommended that individuals with a history of significant allergic reactions should not receive the Pfizer/BioNTech Covid-19 vaccine.
NHS England national medical director Professor Stephen Powis commented: “As is common with new vaccines, the MHRA have advised on a precautionary basis that people with a significant history of allergic reactions do not receive this vaccination, after two people with a history of significant allergic reactions responded adversely yesterday. Both are recovering well.”
The two unidentified NHS workers in question are understood to carry adrenaline autoinjectors – such as an EpiPen or Emerade – which suggests they have experienced prior severe allergic reactions.
How well do you really know your competitors?
Access the most comprehensive Company Profiles on the market, powered by GlobalData. Save hours of research. Gain competitive edge.

Thank you!
Your download email will arrive shortly
Not ready to buy yet? Download a free sample
We are confident about the unique quality of our Company Profiles. However, we want you to make the most beneficial decision for your business, so we offer a free sample that you can download by submitting the below form
By GlobalDataA statement from Pfizer UK said: “We have been advised by MHRA of two yellow card reports that may be associated with allergic reaction due to administration of the COVID-19 BNT162b2 vaccine.
“As a precautionary measure, the MHRA has issued temporary guidance to the NHS while it conducts an investigation in order to fully understand each case and its causes. Pfizer and BioNTech are supporting the MHRA in the investigation.
“In the pivotal Phase III clinical trial, this vaccine was generally well tolerated with no serious safety concerns reported by the independent Data Monitoring Committee. The trial has enrolled over 44,000 participants to date, over 42,000 of whom have received a second vaccination.”
A packaging leaflet for BNT162b2 notes that the vaccine should not be given to someone who is “allergic to the active substance or any of the other ingredients of this medicine”, which include potassium chloride, sodium chloride, sucrose and cholesterol.
In addition, the leaflet makes it clear that, as with any new medicine available in the UK, “this product will be closely monitored to allow quick identification of new safety information”. It encourages anyone who has received the vaccine to report any side effects using the MHRA’s yellow card procedure.
Experts react
King’s College London visiting professor and chair of the Faculty of Pharmaceutical Medicine’s Education and Standards Committee Professor Penny Ward commented: “The prescribing information for the vaccine issued by the MHRA includes a contraindication for use of the vaccine in any individual that is [allergic or] has had an allergic reaction to the vaccine or to any of the components of the vaccine.
“It is understood that the people concerned had a history of allergy severe enough to require them to carry an adrenaline autoinjector; such persons would be at increased risk of an allergic reaction, compared to the population without a history of severe allergy. As these two events occurred in people with a history of severe allergy, it is sensible of the MHRA to draw attention to these reports and to suggest that individuals with a history of severe allergy not receive the vaccine at this time.
“[The] MHRA is actively monitoring the safety of the vaccine during clinical use and can be expected to provide updates to practitioners as more information is gathered. The prompt reporting of these events using the yellow card scheme and the rapid issuing of additional information to guide practice shows that the safety monitoring system is working well.”
London School of Tropical Medicine professor of pharmacoepidemiology Professor Stephen Evans added: “Allergic reaction occurs with quite a number of vaccines, and perhaps even more frequently with drugs. So it is not unexpected.
“The Pfizer data showed that about 0.6% of people had some form of allergic reaction in the trial on the vaccine, but about 0.5% on placebo. So there was a genuine excess of allergic reaction but this was small and the true rate is not known.
What would be wise, as the MHRA have already advised, would be for anyone who has known severe allergic reaction, such that they need to carry an EpiPen [or another brand of autoinjector], to delay having a vaccination until the reason for the allergic reaction has been clarified.
“For the general population this does not mean that they would need to be anxious about receiving the vaccination. One has to remember that even things like marmite can cause unexpected severe allergic reactions.”