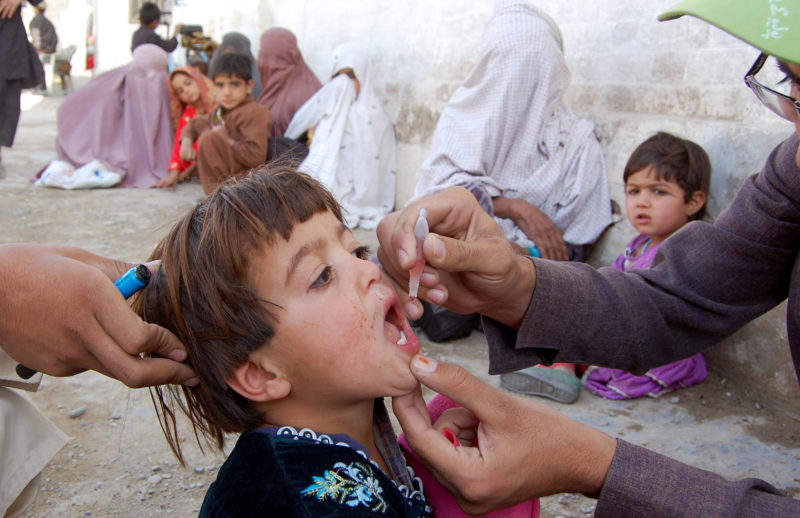
In public health, zero is an important number, and a difficult one to reach.
“This is the number we’re striving toward every day at the foundation,” wrote Bill Gates in 2017’s annual letter updating on the activities of the Bill & Melinda Gates Foundation, the largest private foundation in the US. “Zero malaria. Zero TB. Zero HIV. Zero malnutrition. Zero preventable deaths. Zero difference between the health of a poor kid and every other kid.”

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
The world is making progress in its fight against major diseases; public health campaigns have contributed to encouraging statistics such as the halving of the number of yearly deaths of children under five since 1990. That adds up to 122 million young lives saved over 25 years.
But actually eradicating an infectious disease globally is a rare feat, not repeated in humans since the World Health Organization declared the end of smallpox in 1980. After a concerted, decades-long campaign, the world is on the brink of doing it again.
Last year, only 37 new cases of poliomyelitis (polio) were reported around the world (not including five vaccine-derived cases). These were confined to three countries – Nigeria, Afghanistan and Pakistan – that represent the disease’s last footholds in the world. The fact that hundreds of thousands of new cases were appearing as recently as the last 1980s brings home the scale of the achievement. And the end of polio is in sight.
“Polio will soon be history,” wrote Gates. “A lot of gains in global health don’t get noticed. Polio is different. Everyone is watching. If things stay stable enough in the conflict areas, humanity could see its last case of polio sometime this year.”
With the end of polio in sight, it’s a good time to take a look back at the global campaign to eradicate this debilitating childhood disease.
Polio: scourge of the 20th century
There is evidence of the effects of the polio virus dating back thousands of years; ancient Egyptian carvings have been discovered depicting healthy individuals with malformed limbs, one of the main effects of the paralytic form of the condition, if the virus enters the patient’s central nervous system. Clinical descriptions of the disease started appearing in the late 18th century, but major outbreaks weren’t seen until the 20th century, when improved sanitation in the developed world reduced the population’s natural immunity, which was previously boosted by regular exposure to the virus.
Polio pandemics swept through Europe, Australia, New Zealand and North America through the first half of the 20th century. In 1952, the US recorded around 58,000 new cases of the disease, more than 3,000 of which ended in the patient’s death, and more than 20,000 were left with some form of paralysis. The prevalence of the disease galvanised public demand for a cure, not to mention a new awareness of rights for disabled people as the population of polio survivors surged.
Vaccines introduced
Researchers sought to develop polio vaccines from the 1930s. 1948 brought a breakthrough when a team at the Children’s Hospital Boston cultivated polio virus in human tissue in the lab for the first time. In 1952, Dr Jonas Salk and his team at the University of Pittsburgh developed an inactivated polio vaccine.
After successful preliminary testing and positive results from the Francis Field Trial, which involved 4,000 children, the vaccine was licenced in 1955. Huge public vaccination programmes followed, and by the early 60s new polio cases had dropped from the tens of thousands to the hundreds. The early 60s also saw the introduction of an oral vaccine incorporating attenuated strains of all three forms of polio virus, developed by Albert Sabin. The oral vaccine, cheaper and easier to administer than the inactivated version, would become key to eliminating polio all over the world.
A global campaign
With the vaccines developed but still unavailable to large swathes of the global population, huge vaccination programmes kicked off, spurred on by the drastic decreases in polio incidents seen in developed countries. These culminated in 1988, when the World Health Assembly, together with partners including Rotary International, UNICEF and the US Centers for Disease Control and Prevention, launched the Global Polio Eradication Initiative (GPEI). The initiative brought together fundraisers, public health authorities, scientists and philanthropists with the aim of eliminating polio by the year 2000.
Although the millennial goal was missed, the GPEI set the stage for a modern and highly effective response to polio, and major milestones were hit throughout the 90s and 2000s. 1994 saw the Americas declared polio-free, as well as the last recorded case in China. Europe reported its last case in 1998, and a host of Asian and African countries followed in the years after. Today, only Nigeria, Afghanistan and Pakistan are still reporting new cases of polio.
Distribution challenges
The major challenges of global polio vaccination campaigns have always been logistical and infrastructural in nature. Conditions on the ground – both in terms of healthcare infrastructure and political stability – have hampered aid workers’ attempts to reach every person who needs to be vaccinated. The oral vaccine’s low cost and easy administration has made it vital to the extensive campaigns, but as a live vaccine, it needs constant refrigeration to be effective, which is a challenge in the world’s hottest and most remote regions.
Security concerns have also been a central obstacle. All three of the countries still reporting polio cases share similar incidents of resistance to vaccination. In Pakistan and Afghanistan, the Taliban issued fatwas declaring that polio vaccination was an American-led conspiracy to sterilise local populations, and similar rumours sprang up in Nigeria. These suspicions have led to the murders of dozens of health workers, and conflict remains the greatest threat to the success of the global campaign to eradicate polio.
On the brink of victory
That campaign is now on the brink of victory. New polio cases have been reduced to a tiny fraction of what they were – 37 last year compared to around 350,000 a year in the late 80s. Zero is no easy number to reach, however. In 2011, New York Times journalist Donald G. McNeil Jr memorably described stamping out the last remnants of polio as “like trying to squeeze Jell-O to death”.
But with so many obstacles overcome – some were sceptical that India would ever fully eradicate the disease, but the country was certified polio-free in 2014 – and persistent funding from the likes of the Bill & Melinda Gates Foundation, polio’s days are surely numbered. Only time will tell if Gates’ hope that the world will see its last polio case in 2017 bears out, but perhaps it’s time to allow ourselves to start thinking about the impact of wiping out a human disease for only the second time in history.
“The world will benefit from the electrifying effect of ending a disease,” wrote foundation co-founder Melinda Gates. “The surge of optimism will draw energy and brains and dollars into global health, and that will intensify the fight against measles, malaria, TB and AIDS.”




