On 20 July, the FDA approved GlaxoSmithKline’s (GSK’s) and Medicines for Malaria Venture’s (MMV’s) Krintafel (tafenoquine) for the single-dose radical cure of Plasmodium vivax malaria infection in persons ages 16 years and older. GlobalData also expects Krintafel to obtain regulatory approval from Australia’s Therapeutic Goods Administration (TGA) by 2019. The initial licensures should pave the way for Krintafel to receive additional regulatory approvals in P. vivax-endemic countries, thereby allowing the novel, single-dose aminoquinoline to begin replacing primaquine for the radical cure of dormant liver-stage P. vivax and P. ovale malaria parasites.
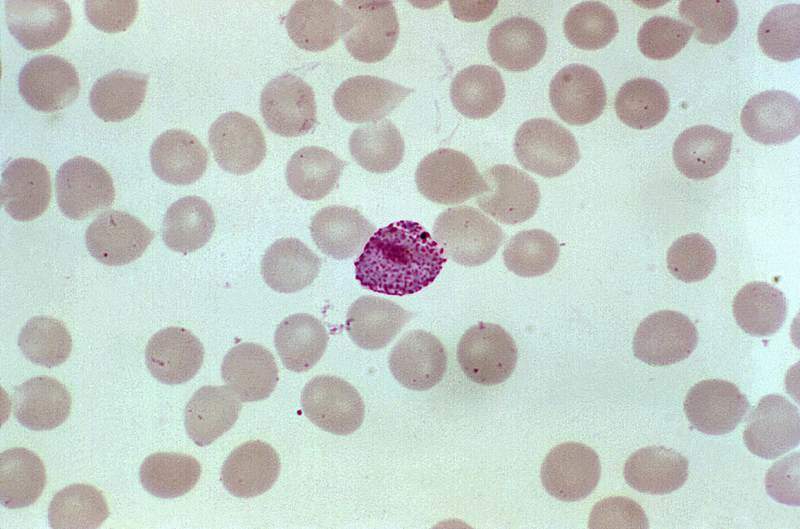
While P. falciparum is responsible for the majority of the 250,000-500,000 malaria fatalities per year, P. vivax is the most dominant malaria parasite outside the African continent, and it is associated with debilitating relapses due to the ability of its dormant-liver stage (hypnozoites) to avoid eradication by most antimalarial agents. Primaquine, which must be taken for 14 days alongside an artemisinin-based combination therapy (ACT) or chloroquine, is currently the sole available treatment for dormant liver-stage P. vivax malaria infection. Given Krintafel’s single-dose treatment course, which will improve compliance, GlobalData expects Krintafel to receive rapid uptake once it becomes commercially available.
According to key opinion leaders (KOLs) interviewed by GlobalData, patient non-adherence to traditional three-day antimalarial drug regimens has contributed significantly to poor treatment outcomes and the growing issue of artemisinin resistance. As a result, experts strongly endorse the development of novel drugs that offer single-exposure radical cure and prophylaxis (SERCaP) dosage capability, which greatly improves patient adherence and helps to curtail the emergence of treatment-associated drug resistance.
Drug resistance to first-generation antimalarial drugs, including chloroquine and others, undermined the first malaria eradication campaign during the 1960s–1970s. The possibility of primaquine resistance is attributed to the observed varying efficacy of primaquine at preventing malaria relapse across P. vivax-endemic regions. Non-adherence to completing primaquine’s 14-day treatment course sets the stage for its drug resistance and represents a key limitation in its ability to prevent P. vivax relapses.
Krintafel meets the SERCaP standard for addressing dormant liver-stage malaria endorsed by KOLs, and its longer half-life compared to primaquine allows for its single-dose full treatment course. Its mechanism of action is thought to be similar to primaquine’s. Krintafel also has label expansion potential for use as a malaria prophylactic, and for malaria parasite transmission blocking for all malaria parasite species, as is currently recommended with reduced dosage concentrations of primaquine.
Krintafel’s regulatory approval ushers in the beginning of the availability of next-generation antimalarial drugs, in the next decade, that will be essential tools to eradicate malaria in the 21st century. In the near future, Krintafel will ideally be paired with antimalarial drugs that provide single-dose treatment for removing parasite blood-stage infection, as is currently done with ACTs. This combination will ensure high patient compliance for achieving P. vivax and P. ovale elimination.