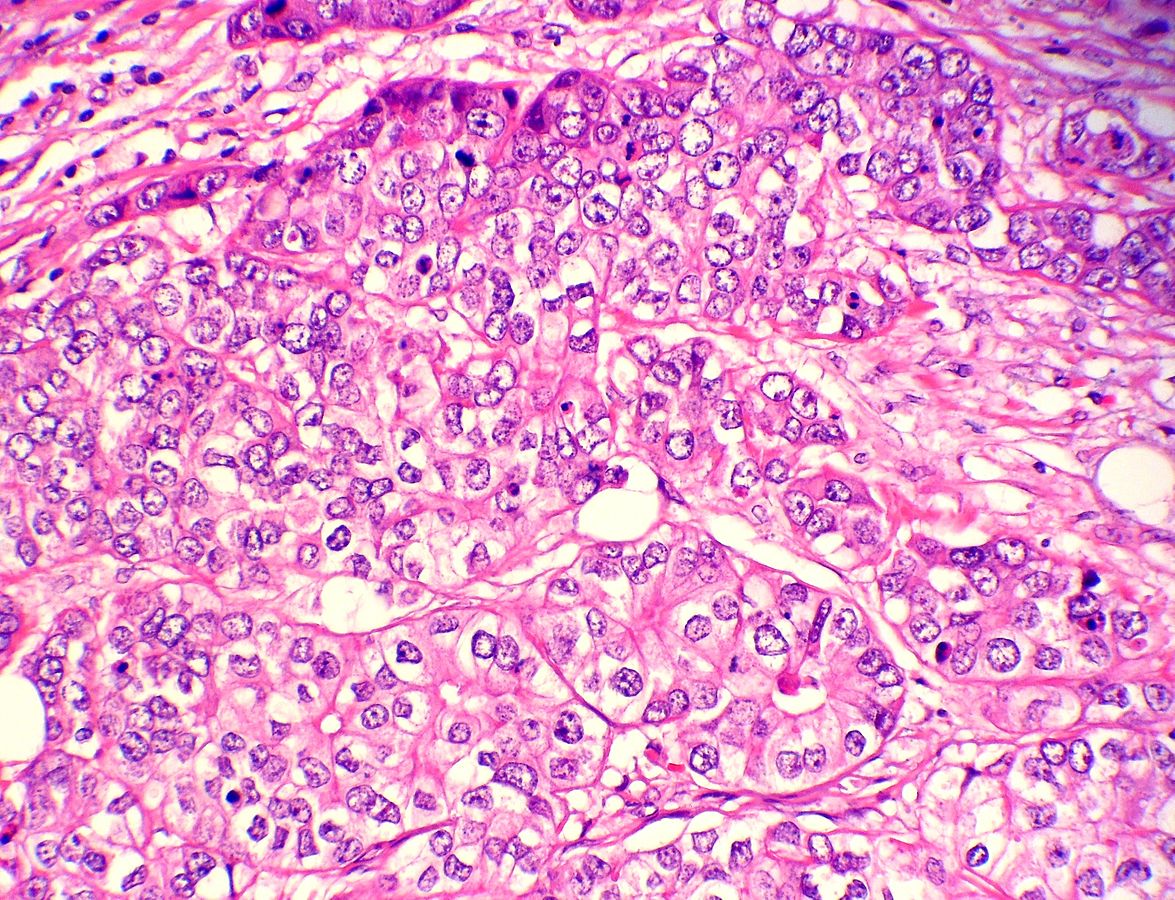
Breast cancer is the most common cancer in women; it represents one in four cancer cases in women and about 12% of all new cancer cases. Approximately two million people were diagnosed with breast cancer globally in 2018, according to the Breast Cancer Research Foundation.
Although breast cancer remains a leading cause of cancer death in both developing and developed nations, World Health Organization statistics show that survival rates in richer countries often exceed 80%. This is primarily due to improvements in early screening, diagnosis and treatment over the past three decades.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Focusing on drugs, most of this success has been in the two most common types of breast cancer – hormone receptor (HR+) and human epidermal growth factor receptor 2 positive (HER2+). HR+ breast cancers express the oestrogen receptor (ER), sometimes as well as the progesterone receptor (PR), and therefore grow in the presence of those hormones, while HER2+ cancers over-express the HER2 gene.
These two sub-types have seen the most progress as drug development from the 1970s onwards has focused on uncovering and resolving the hormonal basis of breast cancer with anti-oestrogen therapies. Moreover, pharma companies uncovered methods of targeting the HER2 oncogene, therefore inhibiting the growth of any tumours expressing that gene.
Unfortunately, this accomplishment has not benefited the breast cancer community equally. Accounting for between 10% and 15% of all breast cancer cases and adversely affecting younger patients of African descent, triple-negative breast cancer (TNBC) cannot be treated with these specialised hormonal therapies or HER2 inhibitors because they do not express ER, PR or HER2.
Unpicking TNBC’s treatment challenges
Not expressing these three proteins and genes has created a challenge in terms of finding the right targets for effective TNBC treatments. The lack of effective, targeted therapies has, in turn, meant that the disease prognosis of TNBC is much poorer than for other breast cancer subtypes.
Instead, chemotherapy is the standard of care for these patients with its multitude of unpleasant side effects. Unfortunately, despite its extensive use both before and following surgery, it is common for this aggressive cancer to return following treatment and spread.
To make chemotherapy safer and more effective in treating TNBC, one approach taken by a few companies has been to design an antibody drug conjugates (ADCs). The first ADC approved for TNBC was Immunomedics’ Trodelvy in April this year.
This method relies on linking a monoclonal antibody that targets a protein expressed by tumours – Trop-2 for Trodelvy – with a highly potent cytotoxic chemotherapy payload – SN38, a metabolite of irinotecan, in the case of Trodelvy. This means that when Immunomedics’ ADC finds a tumour expressing Trop-2 it selectively delivers the SN38 payload to the tumour. This improves both the efficacy and safety of chemotherapy for TNBC patients, particularly in heavily pre-treated patients.
Trop-2 is a very important target for TNBC therapies. However, these patients require more than one weapon in their arsenal and there remains an urgent need to find other druggable TNBC target; researchers at the Australia-based Garvan Institute of Medical Research have done just that.
Leveraging cellular genomics tools, the study identified a potential method that TNBC tumours use to evade the immune system, which could be the key to finding new therapies for this overlooked breast cancer.
Light at the end of the tunnel for TNBC
Using next-generation cellular genomics sequencing, a team at the institute led by associate professor and head of the Tumour Progression Laboratory Alex Swarbrick analysed 24,271 cells from five TNBC patients’
The researchers searched inside these patients’ tumour cells to find out more about both the cancer cells themselves and the immune and connective tissue that supports the growth and spread of TNBC tumours.
By analysing the active genes in the tumour cells, the researchers identified four cell subtypes of stromal cells, a form of connective tissue. The Garvan Institute team dug a little deeper and found the stromal cells’ signalling molecules were interacting with immune cells.
For instance, one of the cell subtypes, known as inflammatory cancer-associated fibroblasts (iCAFs), was found to release CSCL12, a signalling molecule that suppresses the anti-tumour activity of T cells.
“If iCAFs are suppressing T cells in triple negative breast cancer, and we can remove this interaction, T cells will be more susceptible to activation and more likely to attack the cancer,” noted Swarbrick. This may help to explain why immunotherapies, a very effective treatment approach in many different oncology indications, have had a limited efficacy in many TNBC patients.
“One of the things that surprised us was that these new cell types, which we previously thought were benign ‘passengers’ in the tumour, are potentially performing an important function in stopping immune cells from doing their job in targeting the cancer,” states Swarbrick.
A future for TNBC therapies
“Cellular genomics is showing us that what we once thought of as one cell type is in reality a diversity of cell types, which will have a significant impact on how we tailor treatments in the future,” noted Swarbrick.
These findings present “a new opportunity to enhance the activity of immune cells within TNBC”, perhaps by combining immunotherapy with a therapy that prevents an interaction between the stromal cells and immune cells.
To make this theory a reality, Swarbrick and his team at the Garvan Institute are planning to analyse more TNBC patient samples. This will help them to “understand the molecular details of how these cells are impacting on the immune cells, which of them are most important and how they can be blocked,” concludes Swarbrick.
He adds: “We know that molecules in some of these cells can be targeted with drugs that are already on the shelf for other conditions, so there may be potential to repurpose existing medication for this aggressive disease.”




