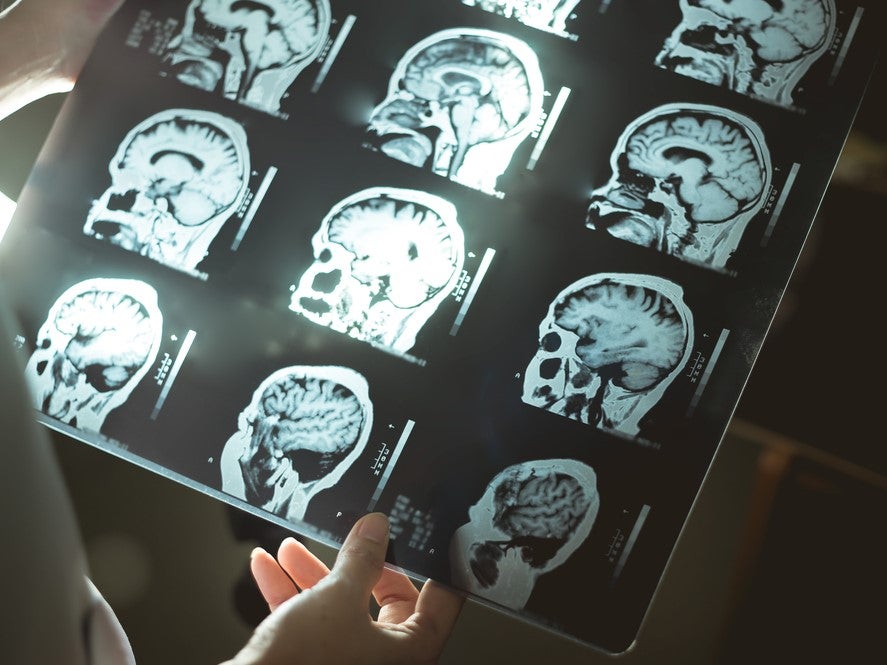
In February 2019, the pioneering GDNF clinical trials programme finally published its full results. A major, multimillion-pound project, which ran between 2012 and 2017, the study investigated whether the GDNF protein might be suitable as a treatment for Parkinson’s disease. While far from clear-cut, the results offer hope to the estimated ten million people worldwide who live with Parkinson’s.
“My outcome was as positive as I could have wished for,” said trial participant Tom Phipps. “I feel the trial bought me some time and has delayed the progress of my condition.”

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Although the study was by some measures disappointing – for one thing, it failed to reach its primary endpoint – the findings are extremely nuanced and do offer grounds for positivity. Parkinson’s UK, which co-funded the study, has described it as a ‘resounding success’.
“Even though the treatment didn’t meet the primary endpoint after nine months, there are lots of other aspects to the study that suggest GDNF was doing quite a lot of good work in the brain,” says Professor David Dexter, deputy director of research at Parkinson’s UK.
How GDNF might work
GDNF (which stands for glial cell line-derived neurotrophic factor) is a growth factor protein that occurs naturally in the brain, and promotes the survival of many types of neurons. When tested in animals, it has been shown to reactivate the nerve cells that are damaged by Parkinson’s, halting the progression of the disease.
As Dexter explains, when the nerve cells affected by Parkinson’s, they don’t just suddenly drop dead – they go through lots of different stages, shutting down various processes once they become sick.
“They almost put their head under a blanket and hope that something is going to come along and rescue them,” says Dexter. “Unfortunately, in the disease nothing is there to rescue them so they eventually die. Growth factors like GDNF can reawaken them, but it takes a little bit of response time to get their former function back.”
Part of the challenge with this kind of treatment lies in working out a route of administration. You cannot simply pop a GDNF pill – rather, the treatment needs to be infused directly into the putamen (a part of the brain responsible for motor function).
In the early 2000s, researchers designed an unusual solution – participants had catheters implanted into their brains, and the GDNF was gradually infused from a reservoir pump in their abdomen. Unfortunately, this didn’t seem to benefit participants, possibly because the rate of infusion was too slow.
In this trial, by contrast, researchers used a specially designed ‘convection enhanced delivery system’ (CED), which delivers a pressurised burst of GDNF into the putamen. This allows a full month’s dose of drug to be delivered in around two hours.
“Unfortunately, GDNF is quite a sticky protein,” says Dexter. “In the past, what they’ve shown is that the drug just stays around the injection site and it doesn’t diffuse across the putamen. With this new delivery system, you can get it to diffuse across the whole of the target area, and that’s a really major step forward.”
What the trial involved
Following a safety pilot with six participants, 35 patients were enrolled into a nine-month, double- blind, placebo- controlled trial. They were subsequently given the chance to continue into an open label extension study, in which all participants received GDNF for another nine months. The study was completed in February 2017, with preliminary results published in July that same year.
Unfortunately, the initial analysis brought bad news – the GDNF group had not performed significantly better than the placebo group. (The metrics being assessed here included motor symptoms and self-reported quality of life.)
It wasn’t until later on, when the entirety of the data had been analysed, that the more encouraging aspects of the trial became evident. From looking at participants’ brain scans, researchers could see that the drug was making an obvious neurobiological difference.
“Researchers did a PET scan that looked at the functioning of the nerve cells after nine months,” says Dexter. “Compared to the placebo group, the treated group saw a 100% improvement on the PET scan. So, while that didn’t translate to a statistically significant improvement in motor function, we’re seeing a vast number of brain cells being switched on at nine months.”
He adds that expecting to see clinical improvements in just nine months was probably quite ambitious.
“If you’re waking up those nerves again, it might take them a bit longer to realise they’re not going to die and they need to start functioning normally – so having a nine-month stop point may be too early to see any clinical benefit,” he says.
Adding weight to this theory, the results from the extension study were very encouraging. Both groups of participants – those who’d originally been on the placebo, and those who’d been receiving GDNF for 18 months – showed moderate to large improvements in motor function. However, these results need to be treated with caution as all the participants knew they were receiving the drug.
Future directions for research
Evidently, GDNF remains a promising avenue that bears further exploration. The big question for the research community is how they can go about this.
“We’re consulting the scientific community about what everyone thinks about the results – is it a strong enough indicator that we should go on and do another trial?” says Dexter. “And if we are going to do one, how should we design it this time to give us the definitive answer about whether or not the GDNF is going to work?”
Any future studies will need to be methodologically rigorous, ironing out the flaws in the original study to give a strong ‘yes’ or ‘no’ result. This may come down to designing better tools for more accurate measures of clinical benefit.
“When a patient goes in to see a clinician for a 30-minute check up, that doesn’t reflect how they are performing in their Parkinson’s throughout the whole day,” he says. “Probably what we’ll need to do is move towards digital capture of data, via sensitive apps on phones and wearable devices that capture a lot of digital data.”
Running another trial will, of course, require funding (Dexter estimates around £3.5m), which may present an additional challenge. However, Parkinson’s UK and the other partners involved are fully committed to exploring the treatment’s potential.
As one final caveat, if GDNF ends up being approved, it is unlikely to be suitable for everyone. The treatment requires surgery to fit a delivery device into the brain, and may strike some people as too challenging a therapy. However, there were no major side effects in trials, and many of the participants continue to report benefits.
“It’s quite an invasive therapy, but the patients tolerated the treatment very well, so it shows you can undergo major brain surgery and derive benefit from it,” says Dexter. “Obviously some people may find this type of approach is not suitable for them. But if we can get the definitive clinical trial done there’s no reason why it shouldn’t be approved as a therapy.”




