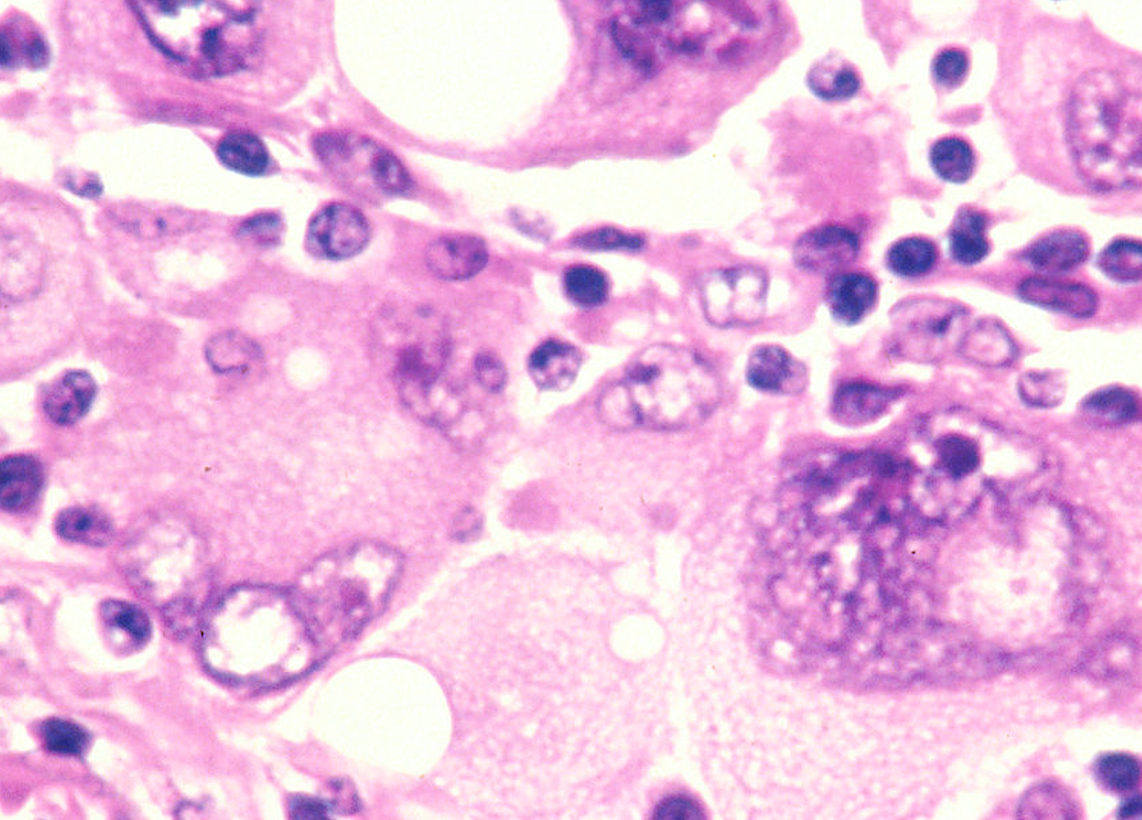
Observed every May, Skin Cancer Awareness Month aims to raise awareness of how the public can protect themselves against this deadly disease.
Skin cancer is the most common form of cancer; according to the World Health Organization (WHO), one in three cancers diagnosed is skin cancer. Around two million people are diagnosed with non-melanoma skin cancers and 132,000 with melanoma every year worldwide, and the incidence of the condition continue to increase.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
The main reason for rising rates of skin cancer is the depletion in ozone levels, meaning more damaging UV radiation is reaching the Earth’s surface; the WHO estimates that a 10% reduction in ozone levels leads to more than 300,000 additional skin cancer cases.
In addition to an increasing number of cases, death rates from skin cancer are also rising. According to Cancer Research UK, deaths from melanoma have risen by 156% in the UK since the 1970s.
This is largely attributed to the fact that the world’s population is living longer than in previous decades. However, the disease is also especially deadly because it is common for skin cancer tumours to quickly become resistant to drugs developed to treat them. One way to reduce skin cancer deaths would be create more effective treatments that can overcome drug resistance.
Understanding drug resistance in basal cell carcinoma
Researchers from Stanford School of Medicine have identified how approximately 20% of basal cell carcinomas, the most common form of skin cancer, remain drug-resistant after treatment with vismodegib, a therapy developed to target drug resistance in this type of cancer. This drug was approved by the US Food and Drug Administration in 2011 under the brand name Erivedge; it was developed and is manufactured by Genentech.
The team, led by professor of dermatology Anthony Oro and postdoctoral scholar Ramon Whitson, noticed that although vismodegib inhibited smoothened receptors of the growth-related Hedgehog pathway, which has previously been found to explain basal cell carcinoma drug resistance, the protein activated by these receptors, GLI1, remained active in the remaining resistant tumours.
GLI1 was identified in a complex with transcription factor serum response factor (SRF), which is associated with cellular scaffolding protein megakaryoblastic leuakaemia 1 (MKL1). Heightened levels of MKL1 were found in the nucleus of resistant basal cell carcinoma tumours, but not in drug susceptible tumours.
Whitson said: “People have long associated changes in the extracellular matrix with tumour progression or resistance to drugs, but this is the first time anyone has identified the molecular causes behind this link.”
Oro added: “Our findings support the idea that tumours have a ‘resistance toolbox’ of mechanisms from which they can choose, based on their microenvironment, that doesn’t depend on genetic mutations often associated with the disease.”
Oro and Whitson thus blocked the ability of MKL1 to increase GLI1 activity using an inhibitor approved for inflammation. This successfully blocked carcinoma growth in mice and in lab-grown human tumours, suggesting this approach has therapeutic potential in drug-resistant basal cell carcinoma.
“Now we know that we can use the presence of nuclear MKL1 as a biomarker to identify patients who might benefit more from MKL1 or GLI1 inhibitors than from vismodegib,” Whitson added.
Repurposing antibiotics for drug-resistant melanoma
Building upon prior findings that the most difficult-to-treat melanoma tumours produced high levels of enzyme aldehyde dehydrogenase 1 (ALDH1), researchers at the University of Edinburgh studied the effect of an antibiotic approved for colitis and diarrhoea, nifuroxazide, on implanted human tumours in mice.
The team, led by Dr Liz Patton, chair of chemical genetics at the Human Genetics Unit, which is part of the Medical Research Council Institute of Genetics and Molecular Medicine, found that nifuroxazide selectively killed tumour cells that produced higher levels of ALDH1, but didn’t damage other cell types.
The antibiotic is designed so it is only activated by ALDH1, and thus only toxic once inside cells producing the enzyme.
Patton said: “When people are given BRAF or MEK drugs to treat melanoma it can result in the tumours having more cells with high levels of ALDH, so we think that’s a really important target. We’ve shown this antibiotic that’s used mostly to target intestinal bacteria can also target and kills cancer cells high in the enzyme ALDH1.”
The researchers think this drug could be effective in combination with BRAF and MEK inhibitors because when they treated cancer cell lines in the lab with these inhibitors, it made them especially susceptible to treatment with nifuroxazide.
Despite optimism about this discovery, the Edinburgh-based team believe more research is needed to ensure this treatment will be effective in melanoma patients. Patton stated: “It’s great that this antibiotic is approved for use in humans, but it wasn’t designed as a cancer drug, so we still need to find out if it’s safe and effective for cancer in humans.”




