Gout is often thought of as an ancient disease, confined to overfed royals from years gone by. One notable patient was King Henry VIII, the corpulent English monarch, who suffered debilitating attacks of gout, as well as a litany of other health problems. Others afflicted by gout have included Alexander the Great, Charlemagne and Queen Victoria.
In 1780, US founding father and gout sufferer Benjamin Franklin wrote a whimsical dialogue between himself and ‘Madam Gout’. “You would not only torment my body to death, but ruin my good name; you reproach me as a glutton and a tippler,” he says to Gout, who reprimands him at length for his overeating and lack of exercise.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Even the word ‘gout’ has a medieval ring. First used around 1200 AD, it is derived from the Latin word ‘gutta’, meaning a drop of liquid. According to the Oxford English Dictionary, it refers to the ‘dropping of a morbid material from the blood in and around the joints’, which supposedly happened when one of the four humours was out of balance.
A growing disease burden
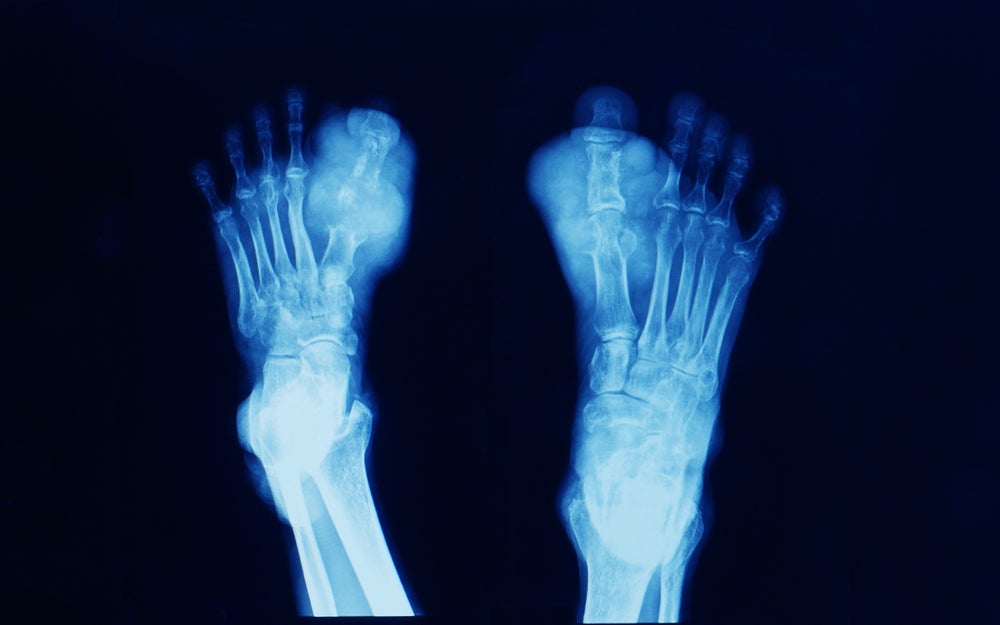
This popular image, however, belies the fact that gout is very much still with us today. A painful form of arthritis, characterised by inflammation around the joint, it is caused by elevated levels of uric acid in the blood. Uric acid crystals build up in the joint, most commonly the big toe, causing sudden, severe pain and swelling.
The disease is thought to affect around 1%-2% of the Western population at some point in their lives, with older men particularly susceptible. In the US, the rate may be as high as 4%.
What’s more, its incidence is rising. According to recent analysis published in the journal Arthritis & Rheumatology, that looked at data from 195 countries, there were roughly 41.2 million cases of gout worldwide in 2017. This included 92 new diagnosed cases per 100,000 people, an increase of 5.5% from 1990.
“The burden of gout was generally highest in developed regions and countries. New Zealand, Australia and United States were the three countries with the highest age-standardised point prevalence estimates of gout in 2017,” says study author Dr Emma Smith, of the University of Sydney. “The trend towards an increasing gout burden is likely to continue as the global ageing population is on the rise.”
Addressing lifestyle factors
As the research confirmed, gout was most common in men and older people (the female hormone oestrogen has a protective effect against gout in women, at least until menopause). High body mass index and impaired kidney function were also identified as independent risk factors for developing gout.
“Increased physical inactivity, excessive consumption of alcohol and certain foods high in purines such as organ meats and seafood could also increase the risk of the disease onset,” says Dr Smith.
Not all gout sufferers are overweight, and not all have a rich diet. As a 2018 meta-analysis made clear, genetics play a far larger role in who develops gout than dietary factors. And in fact the ‘disease of kings’ stigma can be hugely detrimental, in terms of increasing distress for sufferers. That said, on a population level, lifestyle factors certainly play a role in the rise of gout.
“Public health promotion for lifestyle and behavioural changes, particularly for physical activity, consumption of variety of healthy diet and limited alcohol intake, should be encouraged in an attempt to prevent the onset of gout,” says Dr Smith. “Tailoring the disease management to high-risk groups, such as the middle-aged male population, is crucial to preventing the disease onset, and hence, decreasing the global disease burden.”
Existing gout treatments
The good news about gout, compared to most other forms of arthritis, is that it’s treatable.
Typically, patients would need a preventative medication in conjunction with a therapy for managing flare-ups.
On the preventative side, the treatment of choice is usually allopurinol, which lowers levels of uric acid in the blood. Other medications, such as febuxostat, are recommended for those who can’t tolerate allopurinol. When this drug hit the market in 2010, it was the first new gout medicine in 40 years.
In 2015, another drug, lesinurad, was approved for gout patients. Because it has a different mechanism of action to allopurinol or febuxostat, it can be easily combined with existing medicines to improve disease management. However, it was pulled from the American market in 2019 owing to low demand and high costs.
The standard treatments for flare-ups include nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen, colchicine and steroids. Unfortunately, while these drugs are highly effective, they’re unsuitable for many patients.
“A common problem in the management of these patients in everyday clinical practice is the fact they usually have many comorbidities,” says Dr Dimitrios Daoussis of the University of Patras School of Medicine. “Therefore, the use of standard therapy may not be feasible and alternative therapeutic options are needed. For example, patients with gout frequently have kidney or cardiovascular disease and are not good candidates for the use of NSAIDs.”
New treatment strategies
Dr Daoussis’ team thinks adrenocorticotropic hormone (ACTH), could be a good alternative. This hormone, which stimulates the adrenal glands to produce steroids, also belongs to a group of proteins called melanocortins that play a role in immune response. We don’t know exactly how it works in gout, but there may be a dual mode of action – endogenous steroid release and additional mechanisms through the melanocortin system.
ACTH has actually been around as a gout treatment since the 1950s, with interest re-emerging in the 1990s once its non-steroidal functions became apparent. However, it hasn’t been used routinely in most countries owing to cost factors. Dr Daoussis thinks it doesn’t have to be this way.
“In Greece, the available formulation of ACTH is low cost, comparable to that of standard treatment options,” he says. “In our hospital, we have been using ACTH as a first-line therapy for hospitalised patients with gout according to local guidelines. In a retrospective analysis, we found that treatment with this agent was very effective with a response rate of 78% and fast acting, with most patients exhibiting improvement within a few hours. Most importantly, ACTH appears as a safe therapy with limited side effects.”
He recommends that the efficacy and safety of ADTH should be further investigated in a large-scale randomised trial involving high-risk patients. A study of this kind is currently ongoing in his department.
Other potential treatment strategies focus on reducing inflammation. The anti-inflammatory drug canakinumab (Ilaris), which has been approved for various autoinflammatory diseases, has been shown to be effective in preventing gout attacks – but its high cost appears prohibitive.
More recently, researchers at Washington State University and elsewhere have been testing a new way to suppress inflammation. They are targeting a molecule called TAK-1 that plays a role in the body’s immune response, in a bid to create new therapies.
With the prevalence of gout now higher than ever before, and significant unmet need among certain patient groups, medical research in this field is likely to continue apace. Far from being an antiquated disease, gout poses an ongoing challenge to healthcare systems in the 21st century.





