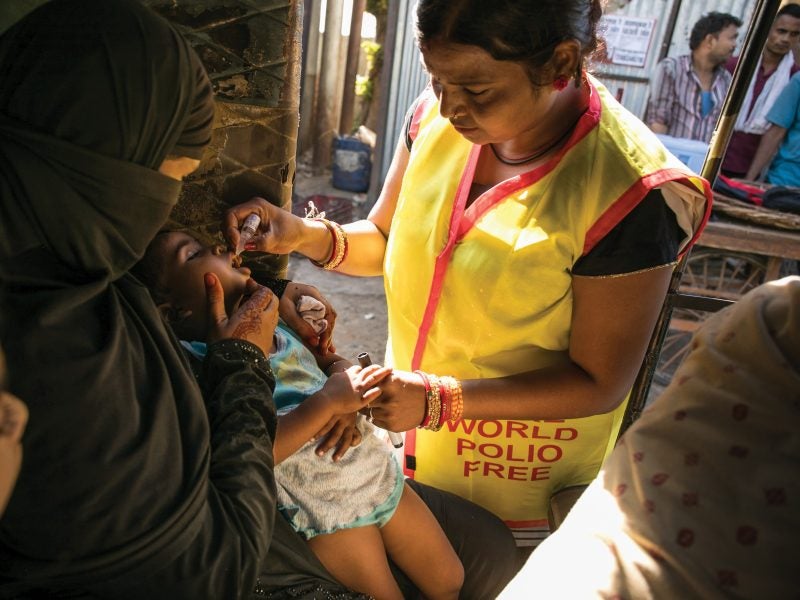
Caused by highly contagious polioviruses accumulating in the gastrointestinal tract, poliomyelitis, commonly known as polio, can lead to muscle weakness and sometimes paralysis; it most commonly affects children aged under five.
Although there is still no effective polio treatment, other than some rehabilitative surgery, there is a safe and effective vaccine to prevent children from contracting the viral infection in the first place.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Despite vaccines against polio being first created in the 1950s, a routine immunisation campaign by the Global Polio Eradication Initiative (GPEI), which was created in 1988, with the inexpensive oral polio vaccine has reduced cases by 99.9% in 30 years. This has been supported by working with local communities and integrating global health and development programmes, such as providing clean water and sanitation to communities to further prevent transmission of the virus.
The Bill and Melinda Gates Foundation is one of the partners involved in creating GPEI; co-founder and co-chair Bill Gates commented: “The world’s progress in fighting polio might be one of the best-kept secrets in global health.”
Although three countries continue to be described as polio-endemic, only two of them – Pakistan and Afghanistan – still have circulation of wild poliovirus. The third, Nigeria, has not seen a case of wild poliovirus since 2016.
In addition, the Global Commission for the Certification of Poliomyelitis Eradication has recently certified that wild poliovirus type 3 (WPV3) has been eradicated worldwide. This makes WPV3 the second WPV to be eradicated, after WPV type 2 (WPV2), and the third human disease-causing pathogen to be eradicated, after WPV2 and smallpox.
World Polio Day, which is organised by humanitarian non-profit Rotary International, one of the GPEI founding partners, aims to celebrate how close the world is to eradicating polio, while also focusing on how failure to achieve this goal could be catastrophic and lead to 200,000 new cases a year. Rotary concludes “no child anywhere is safe until we’ve vaccinated every child.”
Carol Pandak, director of PolioPlus, Rotary’s campaign to rid the world of polio, explains the progress that has been made in eradicating polio to date, the barriers that remain to full eradication and how the polio vaccination programme can act as a model for eradicating other vaccine-preventable diseases.
Allie Nawrat: In 2019, how close is the world to polio becoming the second completely eradicated disease, after smallpox?
Carol Pandak: We’re closing in on a polio-free world. We have certified the eradication of type three polio, which would mean that two types of polio have been certified eradicated.
WPV2 was eradicated in 2015, so that leaves only one strain continuing to circulate – WPV type 1 – and in only two countries; just Pakistan and Afghanistan are reporting cases of wild polio virus. The virulent vaccine [used in the immunisation programme] contains WPV3 and WPV1.
AN: What are PolioPlus and Rotary International doing to safeguard the impressive successes and gains made to date in eradicating polio?
CP: To safeguard a polio free world, the GPEI, of which Rotary is a partner, continues to immunise over 400 million children every year in 40-plus countries in order to sustain high levels of population immunity, because as long as the polio virus circulates anywhere in the world, our children are at risk. So the programme continues to immunise all children under the age of five to protect them from polio.
AN: What barriers remain to the complete eradication of polio?
CP: The barriers that we have remaining in Pakistan and Afghanistan have to do with access to children; some of them are very geographically remote, they’re living in areas of conflict, they’re highly mobile populations as tens of thousands of people cross the border every day. This makes it difficult to make sure you are reaching up to 95% of children in a particular area, which interrupts the transmission of the virus.
Also, there are some concerns of parents about the safety of the vaccine, particularly in Pakistan. The majority of parents want their children to be vaccinated; it’s a very small percentage that have concerns about the vaccine. [This is because] there have been some rumours about the safety of the vaccine.
AN: How is PolioPlus planning to collaborate with partners to overcome these challenges and continue the fight against polio?
CP: We need to ensure that we have the highest quality immunisation campaigns possible in these last few areas. We are working with GAVI, the vaccine alliance to strengthen routine immunisation in addition to the supplementary immunisation campaigns that we do in the GPEI.
We’re working with other development partners to provide additional complimentary services like providing clean water to families. It’s important to have clean water, particularly for handwashing, because polio is transmitted via the oral faecal route.
It’s also important to work with local influencers and community leaders, such as local ulama, who are religious scholars, to promote the message of the benefits of polio immunisation.
What worked very well in India was to make sure that those people that are out there in the communities immunising are recognised in the community. Also, that they’re not only in the community for polio vaccinations, but in between rounds to talk about overall health and why hygiene and sanitation are important, meaning they become a familiar face in the community who people trust.
AN: With effective vaccines now available, has the polio eradication effort now shifted from a scientific effort to a logistical one?
CP: We know we have the tools that can eradicate polio – an oral polio vaccine that can interrupt the transmission of the virus. So now what we’re looking at is logistical; it’s getting that vaccine to children, having high quality campaigns. It is also political; we need political will not only at the national level, but down to the district or lower administrative level of government. Everybody needs to be on board; it needs to be an all-party issue so all of the different political parties are supporting it. You also need financing to fully implement all the activities that need to occur.
AN: Do you think there are still polio treatment innovations that could have an impact on combating the disease?
CP: What makes polio so devastating is there really is no cure; there is only prevention. One in 200 people have the paralysis symptoms of polio and it is particularly devastating if you are living in a remote region in Pakistan or Afghanistan that don’t have the services to help you and a wheelchair is not going to help you get around necessarily.
There is a lot of work going on related to post-polio syndrome. But as polio can be eradicated and we have the tools to do it, that should be the focus as we can prevent the symptoms and paralysis happening to people; and we are very close to doing so.
AN: Looking forward, how can the lessons learnt from the near eradication of polio since the 1980s support tackling of other vaccine-preventable diseases?
CP: The GPEI is a model of how you reach every child with vaccine. We’ve eradicated polio in all but small areas of two countries. When we’re looking at, for example, the measles campaign, they want to replicate that ability to reach every child with the vaccine.
There are [also] lots of lessons about engaging in communities in the effort to eradicate polio, they need political commitments, and the financing to implement the activities that you want to for all other vaccine-preventable diseases.




