New research from the University of Illinois and the University of Iowa has showed that a common antifungal drug, called amphotericin, could help cystic fibrosis (CF) patients fight chronic lung infections.
CF, which is a life-threatening genetic disorder affecting the lungs, is caused by a defect in the cystic fibrosis transmembrane conductance regulator (CFTR) gene.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
CFTR normally produces a protein that channels movement in and out the cells. However, an error in the gene results in a defective protein which causes the accumulation of acidic and sticky mucus in the lungs.
Affected lungs are vulnerable to bacterial infections. Though treatments are available, not all patients respond to them.
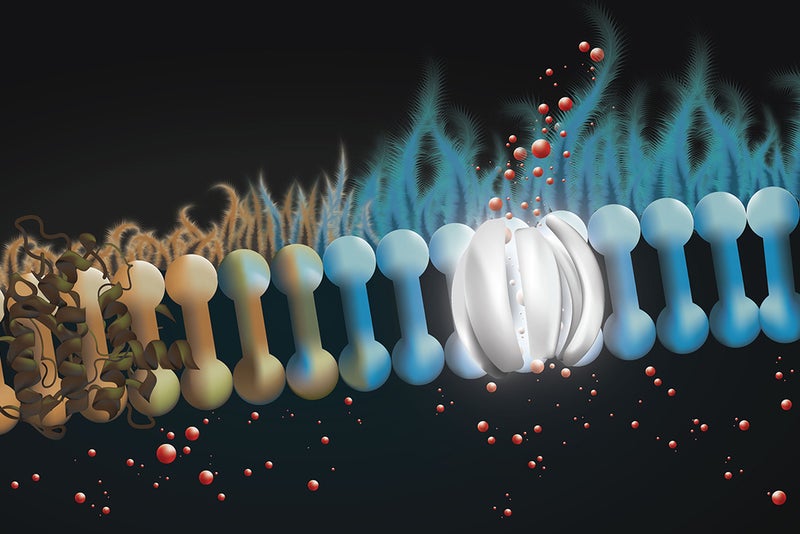
The latest study showed that amphotericin could act as the protein channel that is defective in cystic fibrosis. The researchers said that the drug operates as prosthesis on the molecular scale.
While existing drugs are intended to correct the defective CFTR proteins, the new approach involves formation of new channels.
This offers hope for a new treatment option for all types of cystic fibrosis, particularly for patients who are completely missing the CFTR protein and cannot be treated with corrector therapies.
Study leader Martin Burke said: “Instead of trying do gene therapy – which is not yet effective in the lung – or to correct the protein, our approach is different. We use a small molecule surrogate that can perform the channel function of the missing protein, which we call a molecular prosthetic.”
When tested in human cells and animal models, the drug was able to restore the infection-fighting properties in the liquid that lines the lung surfaces.
The US National Institutes of Health (NIH), which partly funded the study, added that the drug led to restoration of pH levels, better viscosity and improved antibacterial activity, among others.
The researchers said that the drug can be delivered directly to the lungs to avoid common side effects.
Currently, the research team is planning to perform clinical trials for assessing the effectiveness of amphotericin delivered to the lungs in cystic fibrosis patients.


