Researchers at the University of California, San Francisco (UCSF) Diabetes Centre have uncovered evidence to suggest assumptions about the cause of type 1 diabetes are incorrect, meaning existing approaches to finding new treatments for this type of diabetes have been misguided.
Dominant opinion on the origins of type 1 diabetes was the body’s immune system was being overly aggressive and mistakenly attacking healthy pancreatic ß cells. This led to unsuccessful development of therapies to protect and restore ß cells.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Instead, in a study published in the Cell Metabolism journal, scientists at UCSF have found that ß cells play an active role in the onset of type 1 diabetes.
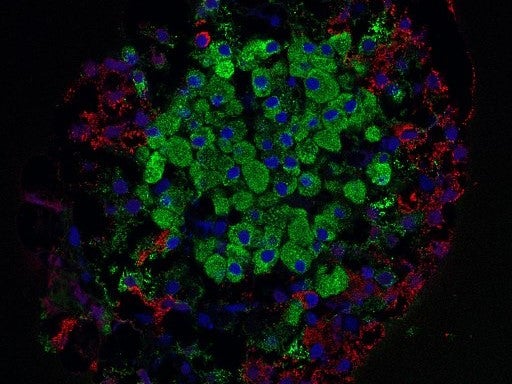
In a study of non-obese diabetic mice, the researchers found that before immune cells attack the pancreatic islets where ß cells reside, the cells exhibit signs of ‘secretory senescence’, a form of cellular decline caused by DNA damage that stops cell functioning.
The issue is that initially the immune system fails to clear out these senescent cells, which allows the cells to spread rapidly and widely. This means that by the time the immune cells actually recognise the problem, they essentially have to destroy the entire insulin-producing system in the pancreas.
Similar results emerged from studies on pancreas tissue from deceased human donors. Signs of DNS damage and secretory senescence were found in the ß cells of six diabetic donors, but not in the ß cells of six non-diabetic donors.
“This discovery is a ‘paradigm shift for type 1 diabetes therapy,” said UCSF Diabetes Centre professor Anil Bhushan.
“The main approach to date has been to dampen the immune system’s attack on ß cells, but this data suggests the problem may not be an immune system gone awry. Instead, perhaps therapies should find a way to do the job the immune system is failing to do: clear the senescent cells early on.”
Postdoctoral researcher at UCSF Diabetes Centre Peter J. Thompson said: “Seeing this data was an incredible moment.
“Many results from these diabetic mouse lines have not panned out in humans, but the fact that we were seeing the very same markers of senescence in human pancreas tissue indicated that the same process is occurring in the human disease as well.”
Consequently, the UCSF researchers tested a senolytic drug approved as a second line chemotherapy for leukaemia, ABT-199 (Venetoclax), to determine if eliminating senescent ß cells could prevent the onset of type 1 diabetes.
Only 30% of mice given ABT-199 for two weeks prior to onset of symptoms developed type 1 diabetes, compared to 75% of control mice who did not receive treatment.
In the 70% remaining mice, their senescent cells were eliminated by the drug and the immune system did not target the remaining, healthy ß cells, meaning the pancreas’ insulin production was not lost.
Bhushan said: “There is great excitement about the potential of senolytic drugs to treat all kinds of diseases of aging.
“Our work is among the first to suggest that clearing senescent cells can also be beneficial in pathological conditions not related to aging, such as type 1 diabetes.”
The UCSF researchers hope that these findings will encourage the development of a therapy that can prevent the onset of type 1 diabetes in young people at risk, as well as preserve remaining ß cell function in recently diagnosed patients.




