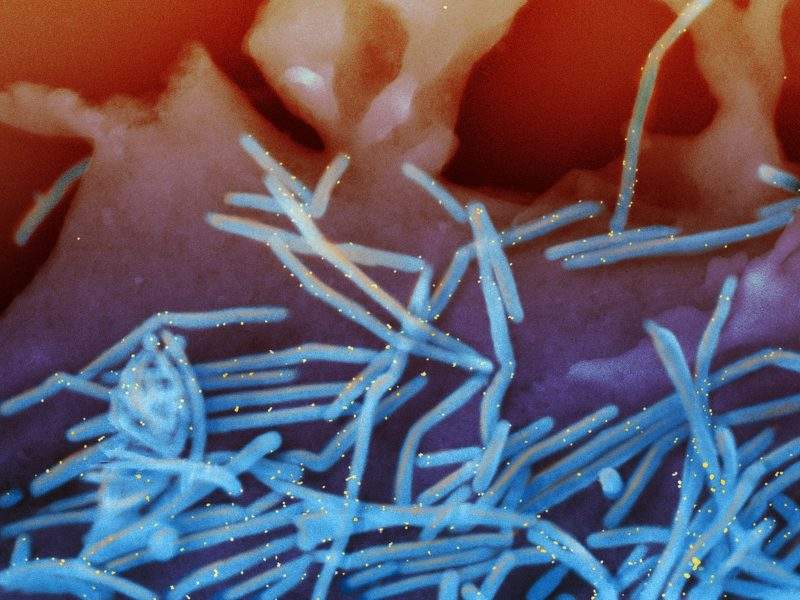
Human respiratory syncytial virus (RSV) is a common enveloped RNA pneumovirus that causes lung and respiratory tract infections. In vulnerable individuals such as infants, the elderly, and immunocompromised adults, RSV infection can be a severe health concern, resulting in lower respiratory tract infections such as pneumonia or bronchitis.
Although Synagis (palivizumab), a prophylactic monoclonal antibody (mAb) for RSV, has been on the market for nearly two decades, there are no approved vaccines for the prevention of RSV infections. On 5 October, speakers at IDWeek 2018 shed light on updates and future directions in the quest for a prophylactic RSV vaccine, placing particular emphasis on preventing infant infection through maternal immunization.
In US children up to five years of age, RSV is responsible for 57,000 hospitalisations and 500,000 emergency room visits per year, in addition to over 1.5 million outpatient visits. RSV accounts for 28% of all acute lower respiratory tract infections (ALRI) in young children, and the vast majority of hospitalisations occur in infants under four months of age. Experts believe that infants are at an increased risk for disease during this period due to a window of low antibody titers, meaning maternal transfer of immunity is the optimal route to confer neonatal immunity against RSV.
However, IDWeek speakers explained that RSV vaccine development efforts have been saddled by inherent and external obstacles. RSV infection itself confers incomplete immunity, and the primary target populations are difficult to design trials around. In an ill-fated 1966 trial, a formalin-inactivated and likely under-attenuated virus resulted in the death of two toddlers from enhanced disease symptoms. More recent research has found that the pre-fusion form of the RSV F protein (RSV Pre-F) can be engineered to stably induce a highly immunogenic antibody response. Some candidate vaccines leveraging this knowledge have moved to clinical trials, which now include live attenuated, vector-based, protein subunit, nanoparticle, and mAb products in Phase I through Phase III.
One promising recombinant vector vaccine from Janssen, Ad26.RSV.preF, is a replication-incompetent adenovirus vaccine using the RSV Pre-F protein as an antigen. It is currently in a Phase I/II trial for adults and RSV-seropositive toddlers, and positioned as a vaccine for RSV-naïve infants who will receive two to three doses of the vaccine at two months of age. Another intriguing product is the Phase II modified vaccinia virus ankara (MVA) vaccine from Bavarian Nordic, MVA-BN RSV, which contains five RSV antigens encoded on a single vector to produce an immune response against both RSV subtypes, A and B.
The most advanced product in clinical development is the Phase III RSV-F nanoparticle vaccine from Novavax. This vaccine is comprised of aggregated RSV-F proteins that form multi-trimer, discrete detergent nanoparticles (20nm-40nm) to induce broadly neutralising antibodies and confer systemic immunity. Novavax’s trial has enrolled 4,600 women across 11 countries in a study to prevent symptomatic RSV lower respiratory tract infection (LRTI) in infants. Experts noted that prior hesitancy about immunisation during pregnancy may not be as much of an issue moving forward, as prenatal influenza and Tdap vaccines are now routinely administered throughout the world.
Adult RSV prevention was also highlighted as is a noteworthy yet overlooked population with unique challenges. For instance, the relatively low incidence of adult infections at 2% to 5% per year creates a recruitment problem for trial design. Some researchers have turned to challenge studies, including one UK study discussed at IDWeek in which 61 adults were inoculated with RSV to study the correlation between nasal antibody levels with protection against symptomatic infection. Another issue is the continuing lack of patient and physician awareness of RSV in adult patients. It is very likely that different vaccine products will be needed for different target patient populations. Finally, once an RSV vaccine is approved for either adult or infant patients, there remain a number of significant financial and logistical challenges to overcome to assimilate an RSV vaccine into existing immunisation infrastructures.