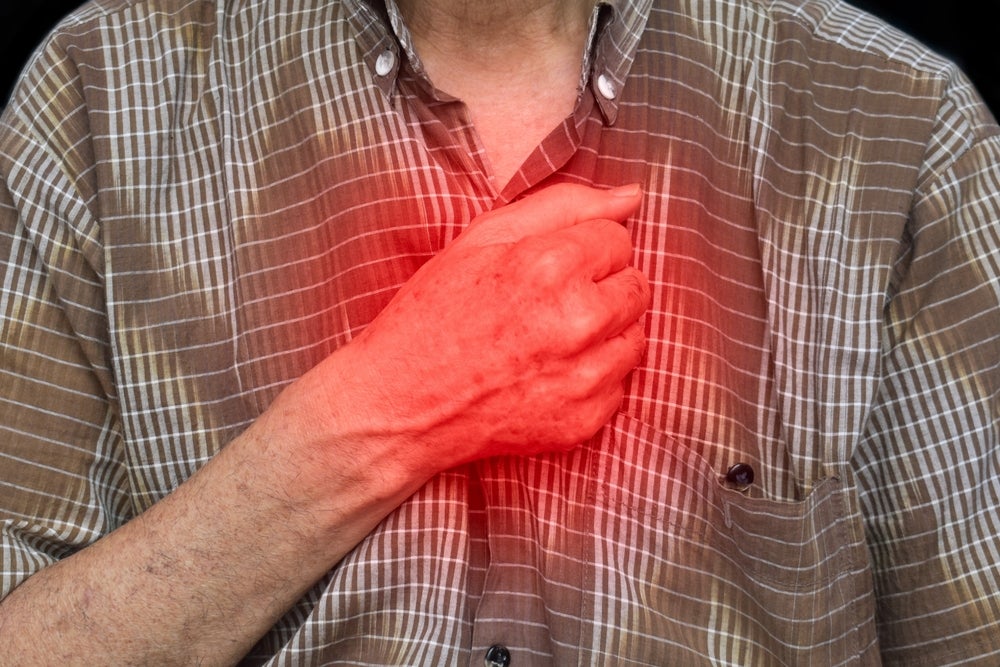
At the 2026 American College of Cardiology (ACC) Scientific Session in New Orleans, the phase II CADENCE trial reported results for sotatercept (WINREVAIR) in adults with combined post- and precapillary pulmonary hypertension linked to heart failure with preserved ejection fraction (CpcPH-HFpEF). This is a high‑risk, older population with no approved, targeted therapies and limited options beyond standard heart failure care.
CpcPH-HFpEF occurs when long-standing HFpEF is accompanied by high pressure in the lung circulation, driven by both lung vessels and the left heart. Patients often remain breathless, fatigued, and prone to hospitalisations despite diuretics and guideline-directed HFpEF drugs, and outcomes are worse than in HFpEF alone.
CADENCE enrolled 164 patients (median age 75 years, predominantly NYHA class III) and randomised them 1:1:1 to placebo, sotatercept 0.3mg/kg, or sotatercept 0.7mg/kg every three weeks for 24 weeks. At baseline, lung pressures and congestion markers were high, and six‑minute walk distance was low, reflecting advanced disease. The primary goal was to reduce pulmonary vascular resistance (PVR), a key measure of how hard it is for blood to flow through the lungs.
Both sotatercept doses improved PVR versus placebo, confirming that the drug can meaningfully ease pressure in the lung circulation in this setting. Additional measures, including average lung artery pressure, measures of left‑sided filling pressure, NT‑proBNP, and time to clinical worsening, also moved in a favourable direction, particularly at the 0.3mg/kg dose, although not all were formally tested for statistical significance. These patterns are consistent with sotatercept having effects on both the heart and lung vessels rather than acting purely as a vasodilator.
A recurring concern with sotatercept in pulmonary arterial hypertension has been a drop in resting cardiac output. In CADENCE, the discussion emphasised that, when cardiac output is considered alongside other measures - improved right ventricular size and function, stable left ventricular ejection fraction, lower filling pressures, and maintained oxygen delivery - the overall picture supports a net cardiac benefit rather than harm. Investigators did not view the cardiac output change as a reason to avoid sotatercept in this population, but acknowledged the need for continued monitoring in later-phase trials.
Dose choice is a central takeaway for pharma stakeholders. While 0.7mg/kg showed PVR benefit, this higher dose had more dose interruptions and discontinuations, often linked to increases in haemoglobin, which may have dampened its apparent effect over time. The 0.3mg/kg dose delivered consistent hemodynamic improvements, encouraging trends in walk distance and biomarkers, and a safety profile closer to placebo, making it the more attractive candidate for phase III development in an older, comorbid group.
Strategically, CADENCE extends sotatercept from Group 1 PAH into a complex HFpEF-related segment where there are no targeted competitors, strengthening its position as a platform asset across pulmonary hypertension phenotypes. The data are still proof‑of‑concept rather than practice‑changing, but they provide a clear rationale for a registrational phase III program and raise the bar for future entrants that aim to serve CpcPH-HFpEF. Success will depend on defining CpcPH-HFpEF in a way that can be operationalised, building diagnostic and referral pathways to find eligible patients, and aligning dose, monitoring, and safety communication with the realities of treating older, multi-morbid individuals.
Looking ahead, the planned phase III program will need to focus on outcomes that matter to cardiologists and payers - such as hospitalisations and clinical worsening - while confirming that the 0.3mg/kg dose sustains benefit with manageable safety and monitoring demands. If those studies are positive, sotatercept could become the first targeted therapy for CpcPH-HFpEF and further reinforce industry interest in activin signalling as a lever in broader pulmonary vascular disease.